|
I wrote this on my personal blog and I thought there may be some expecting runners here that might enjoy it. Of course check with your doctor before running while pregnant or after having your baby. May 28, 2013 On Saturday I went for my first long run since Indy was born. Five miles along the Monterey Bay coastline, I even took on the crazy switchback hill without slowing down. On the drive home I felt amazing, and all kinds reasons why all moms should run kept popping into my head. So.... Why I think moms should run:
0 Comments
Sorry... I was in the mood for alliteration and I just couldn't resist. So a fellow Birth Boot Camp instructor, Alexa Gumm, made a pumpkin muffin that the other BBCI's were raving about. She posted the recipe and it looked awesome... but it was missing one thing... protein! So I decided to play with the recipe and I'm really happy with the outcome. The muffins are moist and rich, eating more than one would certainly be a challenge. I would even give moms with gestational diabetes the green light to go ahead and try this one! One muffin comes out to 7 grams of protein! What you'll need: 4 eggs 1 cup of sugar 1 (16 oz.) can pureed pumpkin 1 1/2 cups Greek yogurt 1 1/2 cups whole wheat flour 1 1/2 cups all purpose flour 2 teaspoons baking soda 2 teaspoons baking powder 1 teaspoon ground cinnamon 1 teaspoon salt 1 package chocolate chips (I use dark chocolate chunks) In a large mixing bowl, beat eggs, sugar, pumpkin, and yogurt until smooth. Add in dry ingredients and mix well. Fold in chocolate chips.
Fill greased or paper-lined muffin cups 3/4 full and bake 16-20 minutes at 400 degrees. I love green smoothies. Sometime I need to feel like I'm really getting a treat though. Enter the pumpkin protein smoothie. Let's just get straight to the recipe so you can drink this thing:
1/2 cup Greek yogurt, plain, look for 23g protein per serving! (vanilla is better than plain here) 2 Tbs milled flax seed (you can leave it out if you don't like the texture) 1 cup of pumpkin puree Medium banana Handful of ice Put in blender... and blend. Drink while you make another because this is what you live off of now. You are welcome. A mom recently asked why successful VBACs (vaginal birth after cesarean) are such a challenge. It's a great question, because they really shouldn't be. A VBAC is just letting the body do what it was supposed to do, a repeat c-section is intervening before that is allowed to happen. But why is it hard to find a VBAC supportive provider, and even when some moms find a provider that will allow a VBAC, why are women with some providers achieving their VBAC goal more than others? Many birth professionals will point to fear and misinformation, and both are completely true... but there is more to the story. Abbey Robinson is a doula, a Birth Boot Camp instructor and is also on the Birth Boot Camp advisory board. She is an ICAN (International Cesarean Awareness Network) support group facilitator as well as the chapter leader of the largest chapter of Birth Network National in the country. Most importantly, she has had three c-sections (two were planned VBACs) followed by an incredible VBA3C (vaginal birth after 3 cesareans). Thank you Abbey for sharing your insight: "This is a very complex answer... I wish it was just as easy as 'fear' In 1996, VBAC rates were higher than ever, when I had my first c/section, as I was lying on the operating table, they were telling me I could have a VBAC... no big deal. ACOG (American College of Obstetrics and Gynocology) says VBAC is safe. In 1999, towards the end of my pregnancy ACOG changed their guidelines to be extremely restrictive towards VBACs. Now all hospitals are required to have emergency services ready for any and all VBACs, an OB had to remain 'in house' for any and all VBACs, I went to my prenatal appointment thinking I could continue seeing my midwife... but no, I had to use an OB. None of my team was suddenly fearful, I had not changed my stance, but guidelines changed and because of that, now I would have a lot more trouble getting the support I needed. What happened? Cytotec happened. Cytotec was being given as an induction drug to VBAC mamas and their uteri were blowing up. literally... babies and mamas were dying. It was horrific. Instead of saying "HEY, stop using that Cytotec on VBAC mamas!"... they said "HEY, VBACs are dangerous!!! We should not be doing them!!" Let me just clarify that the risk of rupture in a scarred uterus although extremely low (about 0.6%-with 96% of those ruptures not causing injury) it's much higher than in a woman who's never had a c/section (even if they are induced, a rupture in a woman with no prior surgery is a freak thing and not comparable to UR in VBACs) NOW... the damage is done. In 2010, ACOG changed guidelines again to be less restrictive, but the impossible restrictions remain in place. In 2005, when I was trying to have a VBA2C, I ended up with crappy midwives because I didn't know of anyone else at all who would give me the chance... that's why groups like ICAN are so important because women can come together and share who truly is and truly isn't supportive.... and it's sad because some of the most NCB (natural child birth) friendly providers just are not VBAC supportive... and some providers who are VBAC supportive are NOT VBA2C supportive... and nearly NO ONE is VBA3C supportive of more... I mean... that is a needle in a haystack. Why? Because it's more dangerous??? NO! Not really at all... it's because ACOG guidelines once again state that VBAC is safe for many women after 1 c-section and some after 2. No mention of 3 or more...we get left off. The risk of uterine rupture is about the same as the risk of cord prolapse, placental abruption... etc... those rare things we talk about that can happen... but NO hospital requires an OB to sit there and wait for a cord to prolapse for a woman who is otherwise completely low risk. VBAC tolerant providers will say they support VBACs but wen it comes down to it, they place impossible restrictions on moms. Its the same basic principle as finding a truly supportive NCB friendly provider, it's just that much harder to find them. Dr. Weinstein gained national attention from all kinds of birth advocates, his posts were being shared by Improving Birth, etc. and he is no longer taking VBACs because of the time it took from his family.... He couldn't survive in the system. It's discrimination and it comes from all levels, most OBs just accept it and push for repeat c-section rather than dealing with the inconvenience of labor sitting. Dr. Cummings (a very VBAC supportive OB) has literally spent his life in that hospital. Sleeping, eating, living there... I honestly don't know why he does it. No one was upset with Dr. Weinstein for stopping VBACs, sad, yes, but who can blame him? Politics, greed, fear, convenience all fuel the lack of VBAC supportive providers but sometimes its just the stupid guidelines and if ONE OB in a practice wants to be supportive but his partners are not... that won't work... that puts a crap ton of pressure on him to be the only one on call for them... and he has no life otherwise. We have to get the primary c-section rate down... those are the jerks we need to go after. I can think of about 5 hospital providers in DFW (Dallas Fort Worth area) who are truly VBAC supportive... maybe 10 if I really dig up the little pockets... but that's it... and that is A LOT for one metroplex area... some places have absolutely zero. We are very lucky here... driving an hour or more to a great provider should be a no brainer if you really want your VBAC.... there are lots more out of hospital providers because they don't have the same stupid restrictions." Having a VBAC is hard not because it's dangerous, but because of a medical system that doesn't understand and often times can't support it. Every subsequent c-section carries more and more risk to mom and baby. Preventing that first c-section is essential! How many women who walk into hospital in labor do you think are thinking "I might be having a c-section today." Not many! If you walk into a hospital with a high c-section rate to deliver with a provider with a high c-section rate who maybe has mentioned the possibility of a c-section a few times you have put yourself on a very slippery slope. If you have already had a c-section the good news is that we do have VBAC supportive providers in the area, but if you have not had a c-section that first birth is the most important in determining what your subsequent births will be like. If you don't choose your provider and birth place carefully you may find yourself in the sometimes difficult position of planning a VBAC for your next birth. Thank you Abbey for sharing your perspective. You are an amazing resource and I'm lucky to know you!  Abbey Robinson serves the Tarrant County, Texas area as a doula and Birth Boot Camp natural childbirth instructor. She is also a group fasilitator for her local ICAN group and a Chapter Leader for the Tarrant County Birth Network. You can learn more about her services and journey as a birth advocate at Divine Birth Doula. My student and friend gave birth to her second baby this week. Her first was a "the works" birth with an IV, pitocin, epidural, infection, episiotomy and vacuum extraction followed by a stay at the NICU for baby. Both births were at Community Hospital of the Monterey Peninsula.
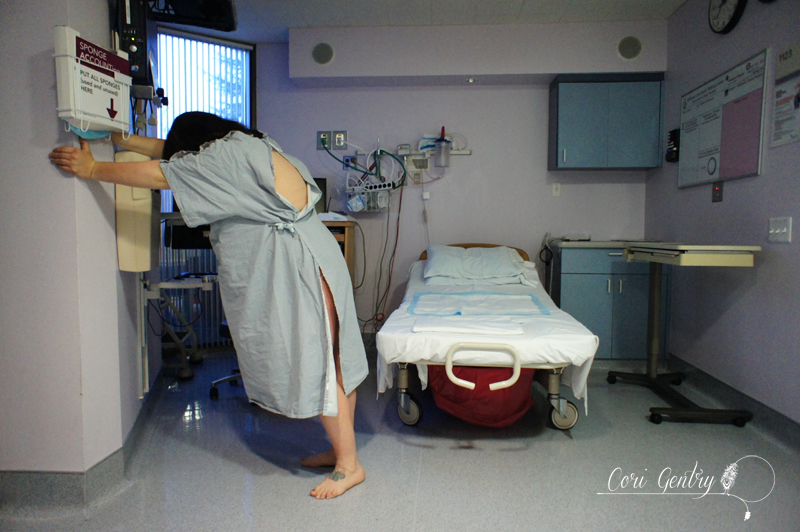
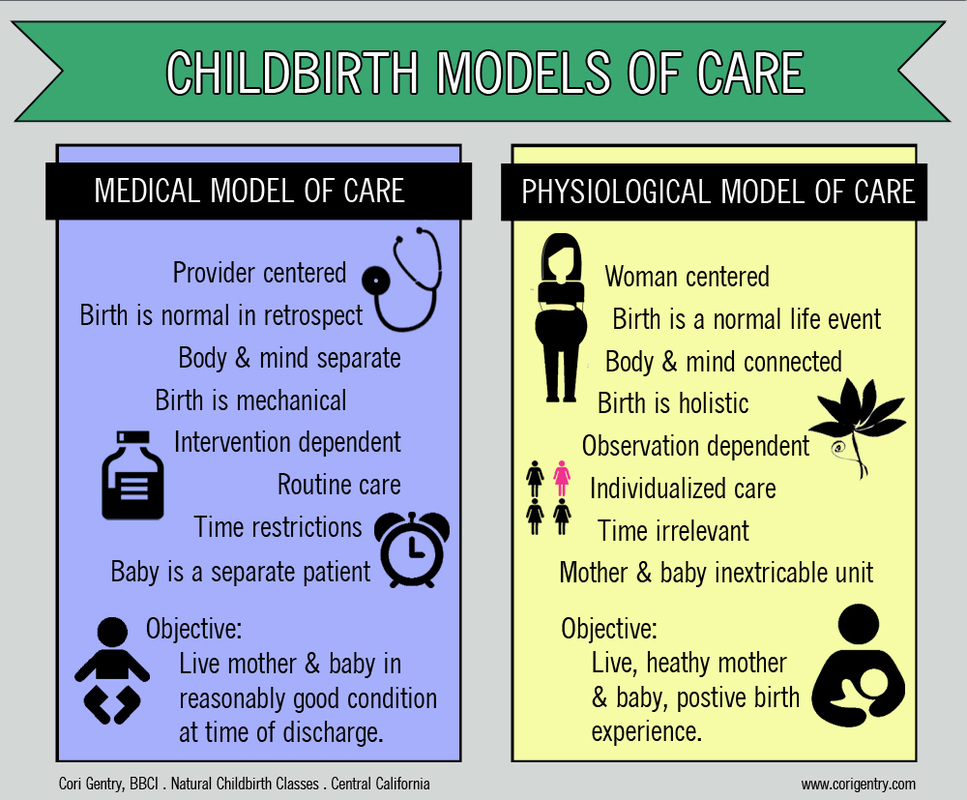
6:09pm, 2 1/2 hours after baby's arrival S: All natural! Me: I'm so proud of you! I cannot wait to hear ALL ABOUT IT!!! IS THERE SOMETHING BIGGER THAN CAPS???? Next morning S: 5 lbs 14 oz.. 19.5 Inches. No tearing or episiotomy.. Baby went right to chest and J cut cord. Me: Well done! What position did you push in? S: I pushed sitting but only because that's what I wanted.. It was only like 5 pushes and she was out. Me: Sitting is still a great position. S: I had the bed at 90 degrees, they wanted me to lay it back. They did offer to break my water at one point.. I was like NO!!!!! But shit that transitional phase was something else.. Ugghhh... Me: Yeah... we don't lie, transition is when everyone is ready to tap out. S: LOL ya I was like I can't do it I can't do it! They were like umm well u are. Me: And was J excited? When I say that Eric gets stoked because he knows we're almost done. S: He was super excited! Dr. wasn't here yet and the nurses were like don't push! I was like too damn bad I can't help it! Water broke as I was pushing and Dr. came in right after. Me: How long were you at the hospital before she came? S: We checked into hospital at 10:30 she was born at 3:23. It literally has been a night and day experience from C's birth. Me: So... you aren't mad I sold you on a natural birth? S: Haha not gonna lie.. I had moments. But ultimately it was much better. The recoop has been 100% times easier already. Me: Good! S: Seriously though Cori.. I am so glad I did it naturally the way it was suppose to be. Best thing I've ever done. So huge thanks to you for getting me the tools I needed to get there! Me: I'm so glad! And portions of this convo is becoming a post right now... S: Yay!! Congrats S+J! It was an honor teaching you and I'm beyond thrilled that you achieved the birth you wanted. And welcome to this amazing, crazy world baby B, we are all so glad you are here! Dominican Hospital is located at 1555 Soquel Dr in Santa Cruz, California. Many Monterey County couples may not even consider Dominican an option because it's in Santa Cruz. Birth according to the movies is lightening fast and perilous, but in reality the first time mother will labor 14-18 hours, leaving plenty of time to travel the 30-45 minutes from Monterey/Salinas to Santa Cruz. Some couples travel much farther, even over state lines, for a birth place that will respect their desires. From Dominican's website: "We deliver small miracles. At Dominican Hospital, we are committed to offering a full service, state-of-the-art, individualized birth experience. Dominican refers to their labor and delivery unit has a "Birth Center." It's important to note that the natural birth experience offered by a freestanding birth center is not the same as the "Birth Center" in a hospital. This is just the name that they have given their labor and delivery. To learn more about freestanding birth centers visit the American Association of Birth Center's website. Dominican is supportive of women who choose to birth vaginally after having a cesarean (VBAC). Many women travel to Dominican to from Monterey for this reason. Dominican's Jacuzzi tub, birth stools, and access to midwives for low risk deliveries may also play a role in that decision. In 2011 almost 450 women traveled to Santa Cruz to have their babies. Out of the total of 926 births at Dominican in 2012, 26.7% of the births were by cesarean section, (www.cesareanrates.com). Though this rate is below the state average of 33.2% and lower than all of the Monterey County hospitals, it is above the World Health Organization's recommendation of 10-15%. Dominican is a non-profit hospital, "a California survey found that women were 17% more likely to have a cesarean at a for-profit hospital than a non-profit" (Optimal Care in Childbirth by Henci Goer). Dominican is certified as Baby-Friendly, meaning they utilize evidence-based practices in the postpartum such as immediate skin to skin, support in breastfeeding, and rooming in. I had my second child at Dominican Hospital in 2011 with certified nurse-midwife Margann Mentor. The nurses were friendly and encouraging, my nurse knew exactly what to say to me when I felt overwhelmed. I could tell they were experienced in working with women who wanted to birth naturally. You can read my birth story here. The following is from a Monterey military mom, Esther: "I can't recommend Dominican Hospital highly enough. They were incredibly hands off through my entire stay, from labor through postpartum. Since I was GBS negative I didn't need an IV for antibiotics and they didn't even ask if I wanted a saline lock. The only needle I ever saw was when they drew blood to bank. I was able to eat while I was in labor and when I did need to be on monitors, they used the telemetry unit so I could still be up and moving around. The telemetry unit is also waterproof so it didn't restrict me from spending time in the jacuzzi tub, which is huge and made contractions so much more bearable I didn't even realize I had hit transition until they did an internal exam. The following are reviews from other Monterey County moms: "I labored in the tub at Dominican and the nurses are AHHHHHHMAAAAZZZZZING!!!! As was that tub! I was in there for quite some time and spent a good chunk of time in the shower as well. I wasn't bothered by any of the nurses and they pretty much left me to labor. Absolutely wonderful! Unfortunately baby had a short stay in the NICU, but fortunately, everyone there was wonderful. I even requested that he receive donor milk instead of formula, as I wasn't getting a drop out of me and the doctor accommodated my wishes! This was my second birth at Dominican and I thoroughly enjoyed that full size bed :0) It was like a vacation. Especially because we were served three celebratory dinners." "Not all OB's at Dominican are VBAC friendly. My frustration lies in the fact that the on call Dr. (Dr. Nicholson) told Dr Klikoff she used the vacuum because they were worried baby's heart rate would dip too low and not come back up and that I wouldn't be able to push him out fast enough. Yet my records say I was pushing very effectively (literally, exactly what the doctor wrote down) and they didn't use the vacuum until he was nearly crowning. Wwwwhhhyyyy?! He was nearly out and I was doing fine! Reading my records just made me even more frustrated than I already was. Another care provider in my doctor's office wasn't surprised at all by his delivery once she saw who delivered him. She said she's far more conservative than Dr. Klikoff...she stopped short of saying she's not VBAC friendly but did say I probably freaked her out, walking into L&D attempting a natural VBAC and already feeling the urge to push." "I was REALLY impressed with Dominican's birthing center tour last night... They highly encourage using the showers during labor if you want... The beds are specifically birthing beds that are designed to have all sorts of bars so you can labor (and push) kneeling, standing, squatting, in bed or out of bed, in whatever position is most comfortable for you. They also have the birthing stools... The sleeper chairs for support staff are a lot bigger and more comfortable than most hospitals, they actually had dads at one of their tours try out a bunch of different models and pick their favorite and that's the one they went with. Of course they have the Jacuzzi tub too that they encourage women to use... "I had a great experience at Dominican with Dr. Klikoff, but I got lucky with a nurse who is at Sutter 99% of the time, and was only covering a shift at Dominican. Her name is Carol and I'm certain she's an angel." "I've had clients deliver there recently and Dominican is fine with eating during labor. They pretty much leave it up to Mom and how she's feeling. You can also bring a few healthy snacks with you--just pull them out when you need/want them." - doula "I delivered there in 2009 - The staff was wonderful, so grateful to the nurses I had!" Reviews from Yelp and Google: "I had both of my youngest children at Dominican - I felt like a queen there. Great, professional staff, beautiful large room, more food than I could possibly eat. I give them 5 stars!" "The birth center has great security, the nurses were nice, the rooms were bright and clean (p/s the post-delivery rooms where you stay for 2 days had double beds, couches, fridges, etc. - way nicer than the post rooms I've been in at Marin General and California Pacific in SF). The rooms didn't feel like a hospital, more like a 2-3 star hotel. Not bad, come on, it isn't the Hyatt. Before the tour I didn't think I would want to deliver at Dominican, now I am 100% happy with the idea. I especially liked how they played 'rock a by baby' on the loudspeakers when a baby is born (it happened two times while we were there), they have a level 2 and 3 intensive care unit for at-risk newborns (which Sutter does not have), and the security is top notch... not that I am a security freak, but it appears to be pretty much impossible to steal a newborn from that ward, the babies wear a low jack type bracelet and there are locked doors with passwords and cameras, etc. That was nice for the hubby who comes from a much more security phobic." "Since the birth of my daughter 5 years ago I have visited Dominican many times. The first was when Dr. Hencke knew what was wrong with me (rare pregnancy complication, which a lot of doctors miss). The whole staff is caring. When my daughter begin having seizures at 5 months old we were in and out of ER and pediatrics till she was one. We had to transfer to Lucile Packard children's hospital twice because, even for having such a great staff, do not specialize in infants and seizures. We had an awful time at LPCH. If I had to pick a hospital (and really who would want to be in a hospital) I would pick Dominican for the caring, compassionate staff." "My son was delivered at Dominican. We were in labor room for 4 shifts, and every staff member we interacted with was amazingly helpful and kind. Same experience in the postpartum section of L&D. Would recommend, 5 stars. Even the food was good." I include every review that is sent to me, if there is helpful information that you would like me to include, please let me know. Learn more about local hospitals and read reviews from local women: Community Hospital of the Monterey Peninsula Dominican Hospital Natividad Medical Center Salinas Valley Memorial Sutter Maternity and Surgery Center You can view and download a chart comparing hospital options and amenities here. Did you give birth at Dominican Hospital? Please share your experience in the comments below! There are two approaches to maternity care: The medical model of care and the physiological model of care, also known as the midwifery model of care. Knowing the different maternity care models and which your provider practices can help you know what to expect during your pregnancy and birth and what your options are within that care model. The Medical Model of Care "Pregnancy in western society, in fact, straddles the boundary between illness and health" - Comaroff 1977: 116 The medical model of care (also known as the technocratic model of care or medical management) is a specific approach to maternity care that both doctors and midwives can subscribe to. If your care provider states that they follow the medical model of care, it's important to know what exactly that means. "Medical management practitioners start from the premise that pregnancy and birth are intrinsically difficult and potentially dangerous process that, when left to occur naturally, frequently result in poor outcomes." - Optimal Care in Childbirth by Henci Goer For care providers that practice the medical model of care pregnancy is a condition that depends upon treatment for a positive outcome. Interventions are necessary and superior to the natural/normal birth process. Some key characteristics of the medical model of care:
The basic premise is that birth is a mechanical process that depends only on "the powers, passage, and passenger" or the strength of contractions, the size of the pelvis, and the size of the baby. No other factors are considered such as the emotional state of the mother, her laboring position, or whether routine interventions are interfering with the labor process. The theory presents that any problem in labor is mechanical and the provider as the mechanic can correct the situation with a procedure or medication. All unwanted effects of interventions are treated with more interventions: "...when high-dose oxytocin infusion leads to nonreassuring fetal heart rate, the medical management model calls for IV fluid boluses, internal fetal monitoring, and, ultimately, cesarean surgery." Optimal Care in Childbirth by Henci Goer This is opposed to lowering the oxytocin dose or avoiding its use in the first place. It is important to emphasize that there is not much space for wiggle room in the medical model. Many providers do try to accommodate women's wishes, but it is a system that is not easily adjusted. For example, a woman who wants the freedom of movement in labor and then chooses a birth place where continuous monitoring is the norm may be thinking, "well, how hard is it to just not hook me up to a monitor?" Very. That monitor is apart of their staff. It reports to the nurses station so that one nurse can be assigned to several mothers. That nurse may not be able to effectively do her job without the monitor. Also, your care provider may be able to access the monitor readings from home or the office, which is a convenience that would be hard to give up. The monitor is also essential to the provider who believes birth is a runaway train ready to fly off the tracks at any moment. Without the monitor, how can a woman labor safely? Those taught under this theory literally may know of no other option. The monitor also reinforces the belief that the baby is a separate patient from the mother needing protection should the mother pursue her desire for a birth experience over the safety of her baby. Refusing an intervention in the medical model of care is not like asking for your burger with no pickles, it's a complicated system and an entire birth philosophy held dearly by its followers. The medical model calls for less time spent assessing the mother as an individual, making this approach convenient for providers. Most routine tests will pick up possible problems in the pregnancy, but at the cost of providing individualized preventative care. For example, instead of looking at a mother's risk factors, family history, and talking to her about nutrition and exercise in early pregnancy, a provider will routinely screen all women for gestational diabetes late late in pregnancy and then treat the women who develop the condition. Treatment may be hard on mom and prevention may have yielded better outcomes, but individualized care is unrealistic in busy practices that see lots of moms. If you are very comfortable with your care provider making decisions for you and you don't mind medical procedures being done even if they may not be necessary, then choosing a provider that follows the medical model will likely not conflict with your personal feelings about birth. If you would like to be apart of making decisions about your care, would prefer a low intervention birth, or believe that pregnancy and birth are a normal part of a woman's life, you will encounter more conflict in this model of care. The Physiological Model of Care “Remember this, for it is as true as true gets: Your body is not a lemon. You are not a machine. The Creator is not a careless mechanic. Human female bodies have the same potential to give birth well as aardvarks, lions, rhinoceri, elephants, moose, and water buffalo.” - Ina May Gaskin, Ina May's Guide to Childbirth The physiological model of care is more commonly referred to as the midwifery model of care, and sometimes woman-centered care. Physiological refers to a characteristic of an organism's healthy or normal functioning (Merriam-Webster Online). The belief held by followers of the physiological model of care is that birth is fundamentally healthy and normal and birth is safest when practices facilitate normal birth. The physiological model of care is a holistic approach that addresses a woman's physical, psychological and social well-being: "The midwifery model of care makes the woman and her life the central focus of prenatal care. A large part of the midwife’s attention focuses on the pregnant woman as a unique person, in the context of her family and her life. The midwife is interested in the woman’s expectations and experience of her pregnancy—her perceptions and beliefs; her knowledge and opinions; her questions and worries; her satisfactions and dissatisfactions; her comforts and discomforts; her desires, decisions, and actions; and the effect of all these on her pregnancy, fetus, labor, delivery, breastfeeding, postpartum recovery, and development as a mother." - Our Bodies Ourselves Some key characteristics of the physiological model of care:
Women who transfer from a provider practicing the medical model of care to one practicing the physiological model of care are often shocked by the differences. Appointments are longer and much more in depth. The provider following the physiological model of care will usually ask the mother what her wishes are in birth as apposed to a women having to ask if a provider will "let her" fulfill whatever her wishes are. Women are an active participant in their prenatal care. The physiological model of care supports autonomy between the provider and mother. In the medical model of care supports class distinctions where the provider holds I higher class standing than the patient. The physiological model of care recognizes that the couple is able to take responsibility for their birth and take part in the decisions that will affect it. Couples are often encouraged to research and care options are thoroughly explained. The woman is not caught in a system where the provider/institution may be biased towards a higher intervention birth which would yield more income for the provider/institution. Holding the perspective that birth is normal does not mean fewer precautions are taken in ensuring a healthy and happy mother and baby. While tests and procedures are not used indiscriminately, all of the tools (like doppler to listen to baby's heart beat, checking blood pressure, ordering blood tests and ultrasounds) employed by those practicing the medical model of care are still used in prenatal visits, but care is taken to ensure all tests are appropriate. The physiological model of care is most often adopted by midwives. While doctors are trained in seeking out complications and intervening in labor, with little or no training in normal birth, midwives receive extensive training in how to facilitate normal birth in addition to being able to identify complications so that mothers who need an obstetrician can receive that care. Middle Ground Model of Care Yes I made that up. Is there a place in maternity care for two models that appear to be so different? A 1999 study distributed a questionnaire to pregnant women regarding their provider style preferences. It found that women preferred elements of both midwifery and medical styles of care." Concluding that: "Broadening access to obstetric care will involve moving from our own preconceived notions of appropriate packaging into a patient-based and multi-option setting for delivery of these services." As women become more informed about our options and the differences between the medical model and physiological model of care many may switch from providers and hospitals that only offer the medical model for providers. This is a positive change for women, and hopefully a wake-up call to those individuals and institutions not practicing woman-centered, evidence-based care. However, hope is not lost for medicine! With cooperation from those who practice the medical model but want to give women options, there is room for both models in maternity care: "Midwifery and medical obstetrics are separate but complementary professions with different philosophies and overlapping but distinct purposes and bodies of knowledge. Physicians are experts in pathology and should have primary responsibility for the care of pregnant women who have recognized diseases or serious complications. Midwives are experts in normal pregnancy and in meeting the other needs of pregnant women— the needs that are not related to pathology. In most countries, midwives have primary responsibility for the care of women with uncomplicated pregnancies." - Our Bodies Ourselves In most of the rest of the developed world in countries like the United Kingdom, Australia, and Japan, low risk women see midwives while women who are determined to need an obstetrician transfer care to one. The result? These countries have much lower rates of maternal and infant deaths... in fact, we are rated 47th. It is safer to give birth in Singapore (3 deaths per 1000 births), Iceland (5/1000), and Qatar (7/1000) than it is to birth here (21/1000). Medicine plays an essential and irreplaceable role in our society, but the medical management model of care alone is an unbalanced system leaving few options for low risk women who hope to have an uncomplicated, normal birth. As an expecting couple you are the consumers. You have a choice in what kind of care you receive. More than just your birth experience rides on that decision. Salinas Valley Memorial Hospital is located at 450 E Romie Lane, Salinas, California. SVMH does not list anything on their website on their amenities, but like our other Monterey County Hospitals, SVMH is certified as Baby-Friendly, meaning they utilize evidence-based practices in the postpartum such as immediate skin to skin, support in breastfeeding, and rooming in. Salinas Valley Memorial provides a level III Neonatal Intensive Care Unit (NICU) and have a perinatologist on staff for high risk births. Out of the total of 1686 births at SVMH in 2012, 32.2% of the births were by cesarean section, (www.cesareanrates.com). Though this rate is below the state average of 33.2%, it is above the World Health Organization's recommendation of 10-15%. SVMH is a for-profit hospital, "a California survey found that women were 17% more likely to have a cesarean at a for-profit hospital than a non-profit" (Optimal Care in Childbirth by Henci Goer). SVMH is one of two hospitals in Monterey County that do not offer the option of vaginal birth after cesarean (VBAC) to women despite the American College of Obstetricians and Gynecologists and The National Institutes of Health's 2010 recommendations to do so. Unlike hospitals who support women in having a VBAC, SVMH is not required to have an anesthesiologist or obstetrician on the floor at all times. In 2011 SVMH had the second highest epidural rate (66%), and the second highest induction rate (20%) in Monterey County*. (Monterey County Weekly) SVMH also does not offer the option to birth with a certified nurse midwife, which is the standard of care in most other developed countries and has shown to improve maternal and infant outcomes according to a recent study including 16,242 women published August 2013 in the Cochrane Database of Systematic Reviews. I had my first child and SVMH in 2009. I found the rooms to be nice, though when I asked for a room with a tub none of the nurses knew which of the two rooms with tubs had ones that worked. One nurse said "no one ever really uses them." I had an IV and ended up not being allowed to use a tub anyway. About half of the nurses were very kind, reviewed my birth plan and were supportive. The other half seemed more interested in monitors and were dismissive of the importance of my birth experience. A few nurses were unkind and and made unnecessary comments. I was given an episiotomy by Dr. Nelson, even though I have gone on to birth a bigger baby by over a pound without even a tear. You can read my birth story here. The following is from a Salinas mom who had five of her six babies at Salinas Valley Memorial. Her first five births were medicated, and I had the honor of attending her sixth and first natural birth. She shares a little about each birth: 1998 - My labor and delivery with Tyler was awful from the time I checked in all the way to the time I pushed him out. L&D nurses were rude and less than compassionate, even telling me at one point to "shut-up there are other laboring women here." When the pain got to the point where I felt I needed pain relief I asked for an epidural only to be told: "Too late, you waited too long so you will just have to deal with it." The OB was Dr. Nelson, not my OB but was in the same group. He was rude, cold and was basically just doing his job. He told me if I wanted this baby to come out faster we should do an episiotomy (which he did). Second baby, first episiotomy! The ONLY positive was that I was able to stay in the same room the entire stay. More reviews from Monterey County moms: "I gave birth at SVMH in April 2013, it was induced so I spent 40 hours in L&D before my baby was born and 3 days postpartum due to my babys' hyperbilirubinemia... "I was 1cm dilated and not effaced at all. They told me to prepare for a long road. They inserted Cervadil and told me to rest up... I wanted to go as pain med free as possible; I really did not want an epidural... "L&D rooms are fairly spacious with full baths [in 2 rooms] for those wishing to use hydrotherapy. Birthing balls are also available, just ask." "SVMH is a baby friendly hospital: they promote immediate skin to skin contact and breastfeeding. Lactation consultant is available during weekdays (I believe) and free breastfeeding support group meets every Tuesday 1 - 2pm. I would recommend calling Shawna, the lactation consultant, Tuesday morning to confirm the meeting. Both times that I showed up I was the only attendee and ended up having a free private consult!" "I was only 3cm dilated which was enough to get me admitted and a bed in labor and delivery. Unfortunately, there were forms to sign and it seemed like it took the nurses hours to get these forms ready. During this time, the contractions were increasing with pain and my mom, my fiance, and I were in this small, dark room with a few nurses watching the tragedy of Michael Jackson on TV. I remember my fiance whispering to me, 'If they don't quit watching that TV we are going to pack you in the car and drive to CHOMP.'" "When I have birthed there (4 times) it was a positive experience with no rush. [With my 4th in 2009] my Dr. at the time anticipated a dinner time baby but I knew better and told him lunch. He was pleasantly surprised. Babies come when they are ready and she was ready before the Dr guessed it." "Our first nurse was HORRIBLE. She took one look at me and rolled her eyes. I had tested positive for Group B strep and needed IV antibiotics to protect the baby during delivery. Apparently the nurse had little patience for this. She gave me the IV, then hooked in the antibiotics, cold. I immediately forgot about the painful contractions. My arm felt like the bones inside it were freezing and breaking apart! It was so painful and unbearable. I begged for some relief. My nurse offered little help... "The labor and delivery rooms were very nice, all the nurses were wonderful. Dr. Chan listened to my wishes (however, I did NOT want staples after my c-section and she forgot and gave me staples....she was very apologetic) My anesthesiologist was the best ever. I did not want morphine and I wanted something for nausea and he was awesome. I was slightly disappointed that the NICU team wouldn't let me see Nathan at birth. I got to hear him cry and they whisked him off to the NICU. I was able to see Adeline and she was much smaller at a different hospital. Recovery was wonderful and Dr. Chan was right there typing her notes while I recovered. That is when she realized she gave me staples and was so sorry. I had to request a breast pump... they kept telling me that I didn't need one yet. They accommodated me but they didn't send anyone from lactation until the next day. No biggie to me since I knew what I was doing anyways. The nurses knew how much I wanted to see my son and got me up there after 12 hours. I didn't get to see Adeline again until over 24 hours. The NICU was wonderful there. We had a private room and that was so nice. Postpartum was awful. Stuffy rooms, super small, no shower. Nursing staff was wonderful... especially Nurse George." I include every review that is sent to me, if there is helpful information that you would like me to include, please let me know. And thanks for the positive feedback guys! "Thank you for doing these reviews, I think they are incredibly helpful for expectant parents." Read about other local hospitals: Community Hospital of the Monterey County Dominican Hospital Natividad Medical Center Sutter Maternity and Surgery Center You can view and download a chart comparing hospital options and amenities here. If you birthed at Salinas Valley Memorial please share your experience in the comments below! Community Hospital of the Monterey Peninsula (CHOMP) is located at 23625 Holman Highway in Monterey, California. Like our other Monterey County Hospitals, CHOMP is certified as Baby-Friendly, meaning they utilize evidence-based practices in the postpartum such as immediate skin to skin, support in breastfeeding, and rooming in. CHOMP provides a Level 2 Neonatal Intensive Care Unit (NICU), babies that are in need of a Level 3 NICU are transferred to a Bay Area hospital like Stanford or UCSF, sometimes to Dominican in Santa Cruz or Natividad in Salinas. CHOMP refers to their labor and delivery unit has a "Family Birth Center." It's important to note that the natural birth experience offered by a freestanding birth center is not the same as the "Birth Center" in a hospital. This is just the name that they have given their labor and delivery, it does not mean they necessarily offer a more natural approach to birth. To learn more about freestanding birth centers visit the American Association of Birth Center's About CHOMP's amenities from their website: What to expect during your birth: "Our 13 rooms are equipped for labor, delivery, recovery, and mother-baby care. As you prepare for the birth of your child, we thought you might like to know some of the things we believe at the Family Birth Center...
In the Monterey County Weekly article, The Holistic Hole, director of CHOMP’s Family Birth Center, Catherine Powers said, "medication-free births like Ellis’s only represent about 1 percent of the hospital’s deliveries. Doulas, though rare, are allowed to attend to laboring moms... We’re all moms here at the Family Birth Center. We believe birth is a choice,” Powers says. “[But] we are a medical model, so that’s what we provide.” You can learn more about the medical model of care (as opposed to the physiological model of care or midwifery model of care) and your options within it here. Out of the total of 1045 births at CHOMP in 2012, 32.9% of the births were by cesarean section, (www.cesareanrates.com). Though this rate is below the state average of 33.2%, it is above the World Health Organization‘s recommendation of 10-15%. CHOMP is a non-profit hospital, ”a California survey found that women were 17% more likely to have a cesarean at a for-profit hospital than a non-profit” (Optimal Care in Childbirth by Henci Goer). Though, in 2012 CHOMP did have a higher cesarean rate than the only for-profit hospital in the county, Salinas Valley Memorial. CHOMP is one of two hospitals in Monterey County* that do not offer the option of vaginal birth after cesarean (VBAC) to women despite the American Congress of Obstetricians and Gynecologists and The National Institutes of Health‘s 2010 recommendations to do so. Unlike hospitals who support women in having a VBAC, CHOMP is not required to have an anesthesiologist or obstetrician on the floor at all times. In 2011 CHOMP had the highest epidural rate (79%), and the highest induction rate (37%) in Monterey County*. (Monterey County Weekly) CHOMP also has the highest episiotomy rate (11%) in the county, which is quite a bit higher than other local hospitals like Natividad (2.8%) and Dominican (2.3%). (CalQualityCare.org) CHOMP does not offer the option to birth with a certified nurse-midwife, which is the standard of care in most other developed countries and has shown to improve maternal and infant outcomes according to a recent study including 16,242 women published August 2013 in the Cochrane Database of Systematic Reviews. The following is a Salinas mom's experience touring CHOMP: I toured CHOMP in spring of 2012. CHOMP seems to only allow pregnant ladies and one other adult on the tour. They also don't schedule a tour until pretty late during pregnancy. I was 6 months (I think) when I finally got to do a tour. More reviews from Monterey County moms: "They took me to my room – which was a teeny tiny room that they haven’t used in a long time but had to shove me in it since they were extremely busy. I stripped my clothes off as fast as I could, got my monitors on and hopped up on the bed. "Being a first time mom, and having heard some negative stories about delivering at CHOMP, I had my concerns about being able to have a natural birth, free from interventions there. However because of my insurance, CHOMP was really my only option. The doctor wanted to induce me at almost 37 weeks because the non-stress test was 94% and they wanted to see 100%. The doc told me he didn't want to have to have me come in every other day for a non-stress test and said I needed to be induced. I didn't have any problems throughout the pregnancy... I've had my 3 kids at CHOMP: 2010, 2012 and 2013. I had gone in the first time expecting to do an all natural birth, no meds. I had an open mind though, knowing and telling myself it would be okay if I did end up getting an epidural. I did and it ended up saving my life and my babies, I truly believe that. I had to be turned on my side and my pelvis/hips slid out of socket because of the weight of the baby and my super lax tendons. If I had not had the epidural, I would have been in immense pain, and not have been able to push. "My daughter was born at CHOMP. We hoped for a natural birth, but one thing lead to another and I got to experience the "cascade of interventions" first hand. We ended up with pitocin, my water was broken, an epidural, episiotomy, vacuum extraction and then my baby had to stay in the NICU for 5 days because of the infection we got while in labor, which I've learned can happen when nurses do many cervical checks after your water has broken." "I had a c-section at CHOMP 5 years ago. I was moved three times starting the day after the surgery. The second room I was in was atrocious. There was a jack hammer breaking apart the neighboring wing. It was so loud I couldn't hear my husband talking nor my baby cry. I asked the nurse if there was anywhere else they could put me and she said 'would you rather be in the hallway?' Anyway, I waited in a wheelchair in the reception/waiting area until a room became available. It took a few hours, but I was grateful, all 13 rooms were full. I went on to have a VBAC at Sutter for my next child." I include every review that is sent to me, if there is helpful information that you would like me to include, please let me know.
Learn more about local hospitals and read reviews from local women: Community Hospital of the Monterey Peninsula Dominican Hospital Natividad Medical Center Salinas Valley Memorial Sutter Maternity and Surgery Center You can view and download a chart comparing hospital options and amenities here. If you birthed at CHOMP please share your experience in the comments below! *hospitals included were those with 200 beds or more
Dear expecting dad,
You are having a baby! Are you excited? Nervous? Have you given any thought to what your birth will be like? Oh wait... what was that? Yes, your birth. I could not have given birth to any of my children with out my husband, Eric. Ok, they would have come out, but it wouldn't have been through my own power. Milo, our first, would have been a cesarean if it wasn't for Eric. When I was scared, he was my courage and reminded me of the confidence I have in birth. When I felt lost, he knew what my goals were and he reminded me of them. When the moment came when the doctor was ready to prep me for the operating room, I looked to Eric first. I needed his guidance in our birth. He didn't have to know a ton about birth, but he knew me and that's why he was so important. Guidance... I know... maybe you were thinking your job would be to just not pass out and guidance in childbirth sounds like it's way out of your birthy skill set. Eric thought so too: I'll be out here... in the waiting room... you let me know when it's ok to look. Don't feel bad, birth is a little scary, the way skydiving and rock climbing are scary, but it's worth it to overcome some of that fear to experience something amazing. There's a lot of talk about the "birth experience." Maybe it's something you've heard your wife say. Why can't you just go to the hospital, have this baby, and go home? Isn't that the whole point - to come home with a healthy baby? Why does how it happens matter? Think about the day you were married? Did you have a big celebration? An intimate ceremony? A private trip to the courthouse? Even if you eloped I bet you have a memory of your new wife smiling back at you in the car. You will never forget that day. Yes, you came away with a marriage certificate, but how it happened is a memory that will be a permanent milestone not just in your marriage, but in your life story. The birth of your child will be no different. You will never forget it, whether it is a good or bad experience. Maybe your wife has already listened to other women tell their birth stories. Women tell their birth stories like they were yesterday, they may only have a few memories that precious. And you know what, if you ask a father and he doesn't just respond with a joke, you'll hear his recollection is just as fresh. Do you want to leave this memory to chance? Protect it. My husband and I took a lot of time to decide what our wedding vows would be. I chose to "love, honor, and obey," and my husband vowed to "love, honor, and protect," and we have lived happily ever after by those promises. However, without having to make a promise in front of his family and friends, a man has a desire to protect his wife and child. Protecting your wife and child does not mean going into your birth ready to fight with your care provider. It is not going into war, it is reinforcing your little home with knowledge and a plan so that when this powerful event blows into your lives you and your wife are not left dazed and hurt. Birth trauma is real, some men and women come away from their births with very painful memories. The quote in the image above is from a documentary that addresses how birth can affect dads called "The Other Side of the Glass: A Birth Film Series for Fathers." The following are two stories of how dads coped with their births. My husband and I are big stand-up comedy fans. Many of our first dates were held in San Francisco comedy clubs. One of our favorite comedians is Louis CK. We are also pretty smitten by Marc Maron, so you can imagine our excitement when the two came together on Maron's podcast, WTF. That interview is actually why this post is even being written. Louis' account of meeting his daughter, me holding back tears in the Target parking lot hurting so much for him and being so proud of him for sharing a story that I know many men carry in silence. Birth is important. How you meet your child matters. Please listen to Louis CK's story below, it's 4 minutes. There is some of language. Listen... I'll wait...
The point of listening to Louis' story is so you can hear his emotion, how important this moment is to him. Isn't is worth preparing for? Protecting? Not just for the safety of your wife and child, that's a whole other post, but for this experience?
The next story is by a friend, Ray. Ray and his wife, Dana, got pregnant right after moving from Pacific Grove to the east coast, which was pretty unfair to all of us they left behind, but we are slowly forgiving them. When Ray asked me what books he should read I listed a few, and since I obviously couldn't offer them my classes, I suggested they take Birth Boot Camp classes online. This is Ray's account of meeting his son, Washington: "I don't know where it began exactly, but I do remember that Jim Gaffigan spurred me on just a little. 'When you think about the male contribution to life, it's kinda embarrassing, really.' That quote and his mention of home birth, inspired me to learn something about childbirth. Dana was carrying the baby, Dana could feel the baby, Dana was going to deliver the baby... I wanted to do something a little more than just stand there, terrified, on game day. I wanted to take responsibility for my wife, especially since this was her first child (meaning she had no idea what she was doing either), and my future baby. I read books. I watched documentaries. I read articles and blog posts. I couldn't do much during her pregnancy, but I could help her be comfortable, healthy, and educated. I took her to a birth class at the hospital. We watched the Birth Boot Camp videos together. I bought lots of books. I tried to feed us healthy food, since I normally cook for us. I encouraged her to walk with me. I did what I could. So, really, congratulations! I hope this was inspiring and not too intimidating. You can do this, you made it through this whole post and that's a fantastic start. Moms, I would love to hear how your partner impacted your birth. Dads, I would love to hear your birth stories! |
 I'm a childbirth educator, birth doula, and birth activist with 4 little boys and occasionally enough time to write. I'm a childbirth educator, birth doula, and birth activist with 4 little boys and occasionally enough time to write.
EventsNatural Birth Series
Sept 28 – Nov 15 Carmel, 6:30–9pm Register Infant Sleep for Expecting & New Parents September 28th 6:30pm - 9:00pm Register Gentle Cesarean: Planning & Recovery September 30th Toro Park, 3-6:30pm Register Natural Birth Refresher October 15th Salinas, 1– 4pm Register Preconception & Early Pregnancy Class October 22nd Salinas, 1– 4pm Register Sibling Prep for Parents & Kids November 4th & 5th Toro Park, 2:-4pm Register Fall Home & Birth Center Birth Series Nov 7 – Dec 12 Salinas 7pm–9pm Register VBAC Class November 12th Salinas, 1–4pm Register Natural Birth Series Nov 29th – Jan 17th Salinas 6:30–9pm Register Archives
January 2017
Categories
All
|