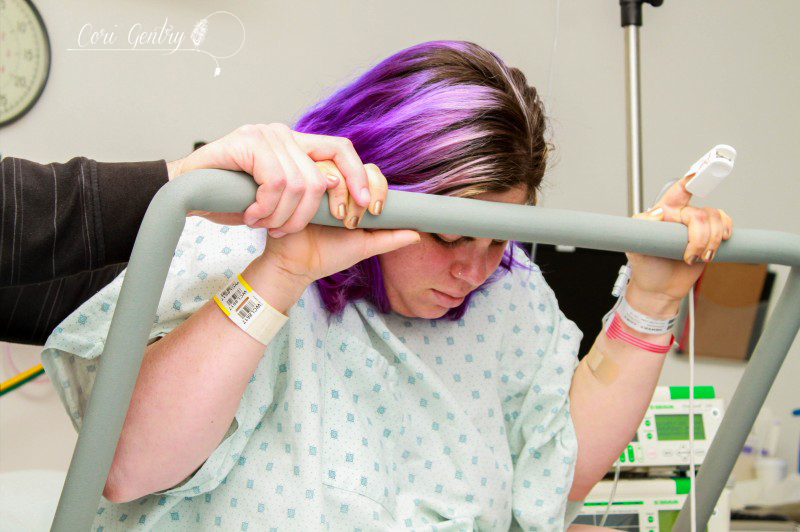|
The key to getting plenty of protein in pregnancy is finding simple meals and snacks. The topping for this is easy to put together ahead of time and throughout the week you can just scoop it onto purchased hummus or make your hummus ahead of time. No cook, that's the key! I love bruschetta. It's what I always offer to bring to parties and potlucks... mostly because I want an excuse to make and eat it. After making a platter of bruschetta for our Birth Boot Camp sip & see I had a bowl of topping left over so I decided to top my hummus with it. It was amazing. Protein: 16g.
You'll need: A roma tomato, chopped Fresh basil Parmesan cheese Minced garlic... like... about a teaspoon I guess Extra virgin olive oil, enough to drizzle 1/2 cup of hummus A couple whole wheat pitas cut into wedges Small squeeze of lemon juice Salt & pepper... to taste This is super easy to toss together. Chop up your tomato and basil. Sprinkle some parm over the top. Stir in garlic and a little evoo and a small squeeze of lemon juice. Add salt and pepper if you wish. Toss. Pour over hummus and drizzle a bit more evoo. Enjoy with pita, but also great with veggies!
0 Comments
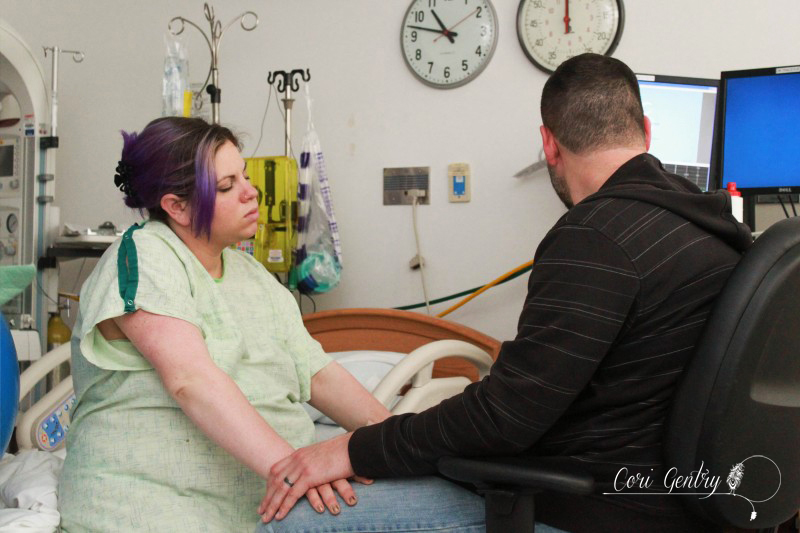
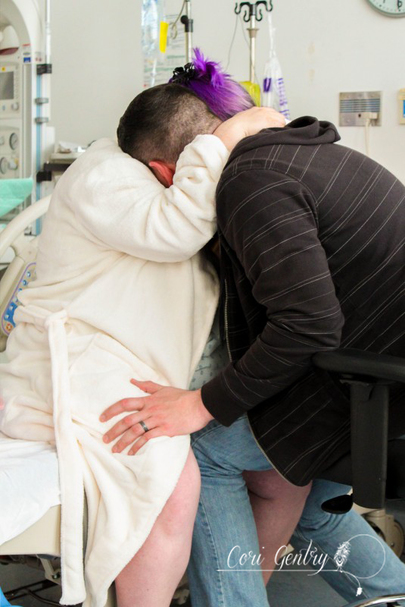
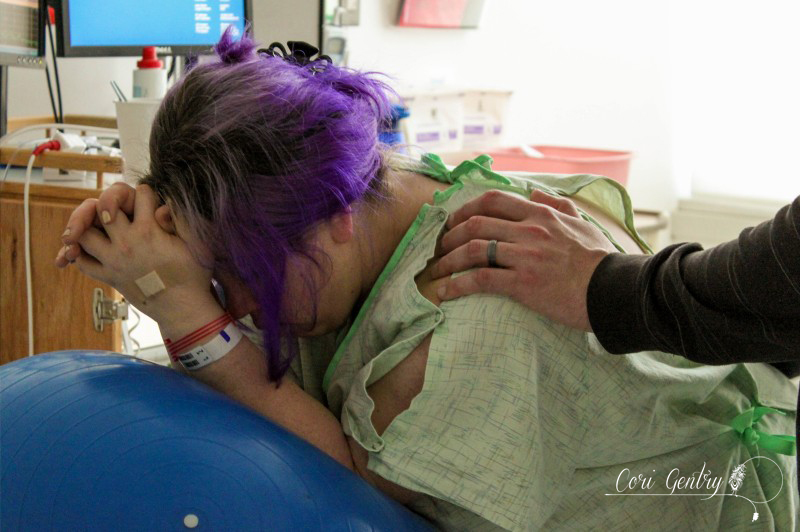
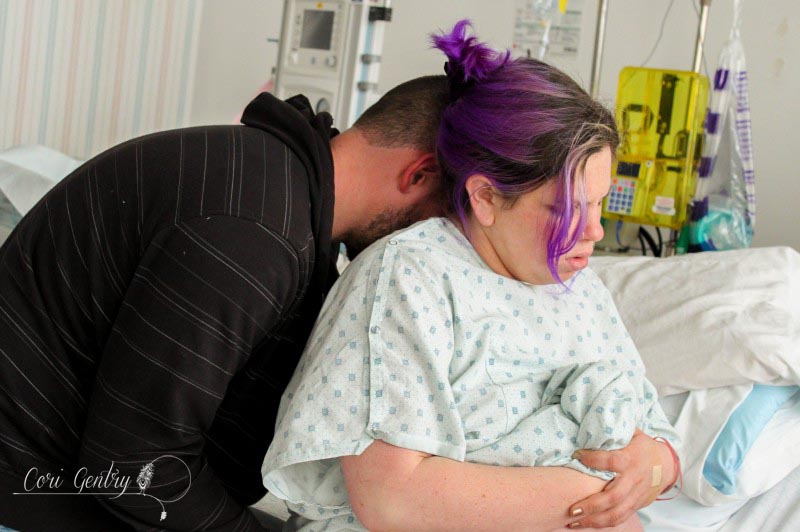
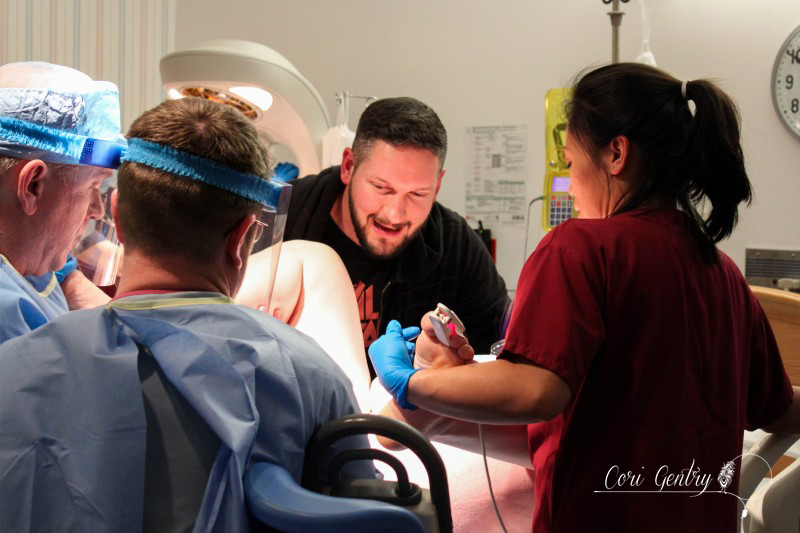
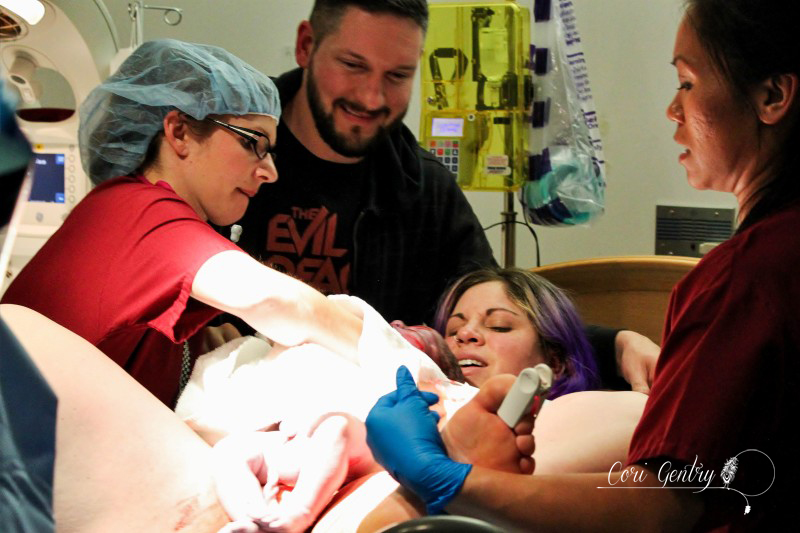
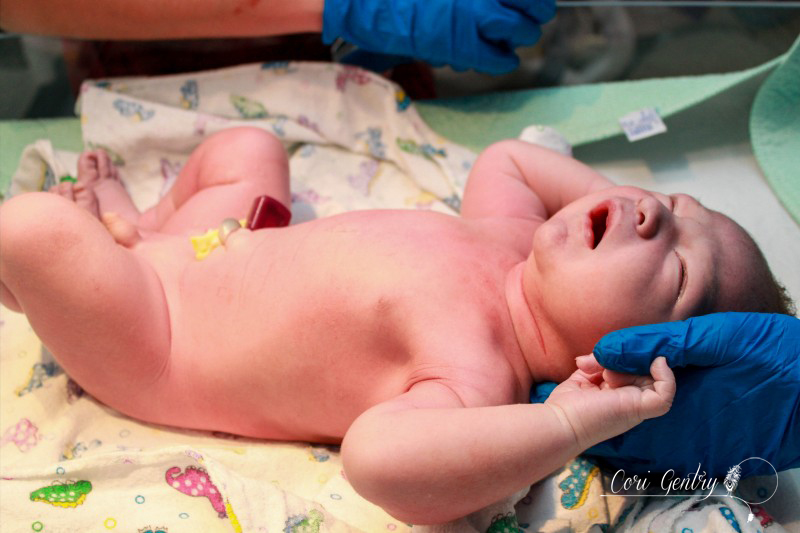
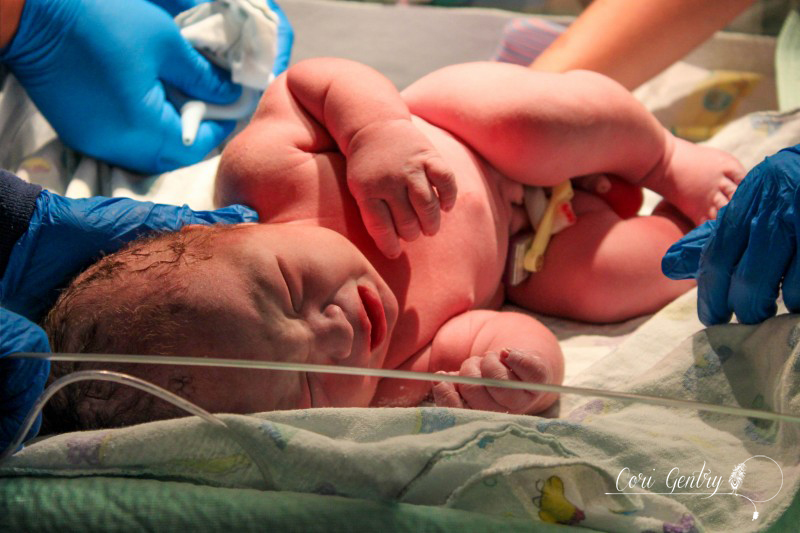
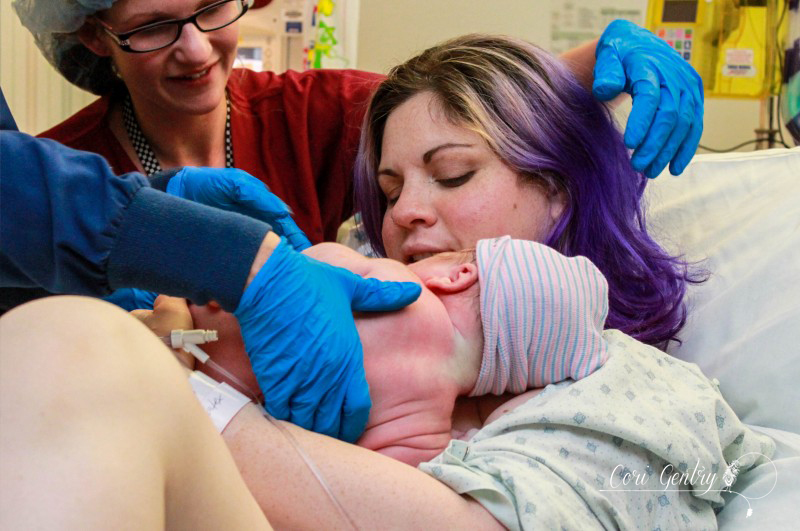
Eric wanted to title this "Indiana Gentry and the Womb of Doom" but since he already got to name our baby Indiana, I'm going to at least draw the line at my uterus being referred to as the Womb of Doom. Here is the story of how we met our third baby, Indy. I wanted very much for this birth to begin spontaneously. Despite having gestational diabetes for the third time, it was completely diet controlled and my doctor, midwife, and I believed baby was not overly big and that we were both healthy. However, as 42 weeks came and went it looked like an induction may be the best option for me considering my medical history. We had a 9:00pm appointment for February 22nd, 42 weeks and 1 day, but Natividad Labor and Delivery called and said their rooms were full. They'd call us when they had space. We heard from them again just before midnight. The first doctor we saw was a resident, Dr. Davis. She explained that she was a doctor of osteopathic medicine (DO) and I immediately felt more comfortable with her. I didn't know much about DO's, but I did know they were more hands on like a chiropractor or midwife. She was the first doctor to palpate my belly during my exam. She felt my head and throat and did a cervical check. I was 5cm dilated, 50% effaced, and baby was -1 to -2 station. Her recommendation was to start Pitocin at a low dose and I agreed, aby was too high to break my water. I requested an anesthesiologist to place my IV since I am sensitive to blood and needles and needed someone who could be quick. A nurse anesthetist was sent in, not the same but whatever. The first thing she did was mock me for having tattoos but being sensitive over needles. Again, not the same... but whatever. I should have sent her out then but I didn't. She placed the IV and said, "see, it's ok to look" but I looked up at Eric instead and he shook his head no. She then realized that she needed to replace it, I started to feel dizzy and said I needed a break. She gripped my hand and started looking for a vein and I said no, I needed some time. She didn't let go right away, but eventually did, maybe irritated over the fact that she wasn't allowed to complete her challenge. Some medical professionals seem to forget we are people, not puzzles. An hour later I was ready to try again with another nurse. She placed the IV quickly but it was excruciating. I started to feel like I was going to pass out and I told her to remove it. Eric and I decided to walk for a while so I could calm down. Back in the room we met another doctor, a fellow, Dr. Rushton. She simply introduced herself as Jill, she was a very calm presence. She thought I was a little less dilated, 4cm. I told her we wanted to think about our options a little more. It had already been a long night so Eric and I rested a bit. I eventually got up to walk by myself while Eric slept. My nurse, Ruby, stopped me in the hall and said that we could just go ahead and break my water. I think she and the doctors knew that I was going to have a very hard time attempting an IV again. My friend Anna arrived. She was interested in becoming a birth photographer and doula and my birth was going to be her first other than her own to attend. She was visiting family in Fresno and drove three hours in the middle of the night to be with me. It was wonderful to not only have a friend but someone else who loved birth with me. Dr. Davis and Dr. Rushton came in a little after 7am. They discussed who was going to get to break my water, then Dr. Davis was called out so Dr. Rushton won. There was no big gush like I experienced in the past. Even when I stood there was only a small trickle. I'm not sure which happened next, if Anna and I started walking or if I took a nap, but both happened. I thought I had napped forever, but it was only around 30 minutes. Despite being exhausted I was anxious to get labor going. I knew a lot could go wrong between a rupture and birth. I woke Eric and told him we needed to do this. Once we were walking contractions picked up immediately and were about 4-2 minutes apart. I hated the feeling of having my water broken. Compared to my first natural birth where my membrane remained intact for most of my labor, these contractions were much stronger and even between contractions my whole pelvis was achy and uncomfortable. Despite the intensity I was encouraged that it looked like I wouldn't need Pitocin. When contractions came I stopped and hung on Eric, it was the only place I could somewhat relax. I focused on trying to let my belly hang the way I did in our second birth but no matter how hard I tried I couldn't quite get to that level of relaxation. About two hours in, around 11:00am, my body began to bear down at the peak of contractions. I told Anna and Eric and they both said I sounded like I was pushing. I had felt this before, twice, and both times I was complete. Could we be there already? I told our new nurse, Caren, and asked if I should get checked and she said she wanted to monitor the baby and my contractions first, we had agreed to monitor for 20 minutes of every hour. The contractions on the monitor were irregular and didn't look strong, but they felt overwhelming. I couldn't lay down, all I could do was sit on the edge of the bed and hold onto Eric. By noon my contractions were no longer building and peaking. I would get a very short indication one was coming and no matter how much I relaxed or panted or fought it, my body bore down with more intensity than I had ever experienced in my life. And not once, but three, four times in one contraction in varied intervals. I tried to maintain control through vocalizations but my moans were lost and I began whimpering sometimes screaming in pain. At noon I was checked. I had fully effaced but I was still only 5cm and baby was -2 station. I was devastated and confused. I was terrified of these contractions. They were unpredictable and unlike anything I had ever heard of. I didn't know what I could do other than to get out of my head and just figure out how to work with them as they came. This is the birth I was given and I was meant to do this. I sat on the edge of the bed and tried to relax as deeply as I could using Eric as support. I was so tired that I could almost fall asleep between contractions. I tried to stay as out of it for the early part of each contraction and not respond to the urges, but I lost every single battle and my body would begin its frantic heaving. I thought maybe the shower might help relax my body. I got in and Eric held my hand from just outside. I panicked if he wasn't in arms reach. I was able to focus on the water and be calm a little longer into each contraction, but each one still ended in frantic pushing. I kept looking down expecting to see blood or something awful. I felt like my body and the baby were crushing each other. Occasionally something in my pelvis popped or cracked at the peak of a push, I was sure either baby or I would be horribly injured. Everything that happened built upon my fear. I know of so many variations in labor and this was nothing I had ever heard of. I don't remember when I started to let myself cry, I was just so scared. Jill, my midwife, arrived while I was in the shower. I don't remember if I even said hi when I came out. My brother, Jon, and his fiance, Lauren, came in too. That morning Lauren had said she wasn't coming and I didn't think my brother would want to so I was surprised, but too out of it to address it. I guess Eric had texted them again. I tried some more positions: leaning on the ball, on my hands and knees, lying on my side. While on my side my hip popped loudly again, Eric heard it too. He said I looked terrified and asked what did that. It felt like I was breaking. I sat on the edge of the bed and held onto Eric. Sometimes I would try to lean onto the bed because I was just so tired, I wanted to sleep, but I would bolt up in pain even if there was no contraction. Jill tried to prop pillows for me but I had to keep my torso totally upright. I could stand or sit straight. By 3:00pm I knew in my head something had to be terribly wrong. I asked to be checked again. I believe I was 6cm, but baby still hadn't come down at all. Baby was not descending despite the immense pressure my body was putting on it. When I told Eric I couldn't do this he reminded me that I already was. He knew exactly what to say. He, Jill, and Anna reminded me to eat and drink, made position suggestions, encouraged me, working as a web to support me. But they didn't know what was happening inside me. I started telling them they were all wrong, I wasn't doing this, something was wrong. I was on my hands and knees crying and Eric got in my face. I said something had to happen, I'm scared, something about my body is not right and I can't stop it. I need something to stop it. I knew an epidural was an option to relax these urges so baby could come down, but that meant IV, a blood test, and an entire route I desperately didn't want to take. Even when I was screaming not a single nurse or doctor suggested pain medications. I let myself say I needed an epidural... Eric asked if I was sure and the nurse reminded me it would be at least 30 minutes for the blood test to get back. I said no, I don't want it, I'd get back in the shower. Minutes in I realized there was no way around it though. We had to do something to stop what was happening. Eric got that this wasn't giving in, we needed to do this. I asked for Fentanyl before the nurse started the IV. It worked. It made me dizzy, as I knew it would, but it helped me get through the blood draw and IV. I don't know how he did it, but the anesthesiologist was able to place the epidural between contractions. Even through my fog I was worried about what would happen if I began bearing down with a needle navigating my spine. The nurse said it would take about three contractions for it to take full effect. By the fourth contraction I felt baby descend. It had only been about 20 minutes. I was still pushing a little with every contraction, but much less and it was easier to resist the urge. I was checked, baby was 0 station and I was complete. I could push. As baby descended some pretty worrisome heart decelerations came up on the monitor. Another DO, Dr. Zwolack, came in and explained to me what has happening, but I knew. He didn't want to say it and I didn't want him to, but I needed to push this baby out or we needed to do a cesarean section. The conversation was not a threat, I really felt like he wanted me to have the vaginal birth I wanted. I was given oxygen and started pushing. Baby was not staying on the monitor so the doctor asked if he could put a monitor on the baby's head and I agreed. I tried a few pushes on my back and on my side. Dr. Zwolack wanted me to push only every other contraction so that the baby had more time to recover. This didn't last long and it was decided that I needed to push baby out. The doctor left and I asked the nurse for the squat bar. I barely felt numb and had no problem supporting myself. One contraction and three pushes and I was able to push baby to a near crown. I'm not sure I could have effectively brought baby down lying on my back. Dr. Zwolack was immediately called back in. The doctor checked again, and I believe the OB, Dr. Heiner, came in as well. Whoever checked me was impressed, none of us knew if I could bring this baby down or not. I got on the bar again and pushed the baby to a crown. I reached down and felt a soft squishy head, squishier than I expected. The OB said that a caput had formed, some swelling in the scalp from being pressed against my cervix. From here everything, and everyone, moved quickly. Dr. Heiner said they would not use a vacuum. If nature could not bring this baby down they would not force it, and I understood completely. That meant I pushed this baby out or they would do a c-section. No pressure. Baby was having a hard time for a reason and we did not know what that reason was. As the room filled the doctor explained there would be more people in the room than previously expected because baby was struggling. I sat back and pushed. There was so much excitement in Eric's voice as he told me I was doing it and the head was right there that I knew I must have been really doing it. There were lots of voices encouraging me and I needed every one of them. It did not feel like I could get baby out. I had to lay back all the way, not how I envisioned birthing this baby, but I wasn't being forced to do anything that I didn't think needed to happen. I think both doctors had their hands in me stretching and maneuvering. I heard Dr. Heiner say to someone he was going to drain my bladder to make more room and the birth fanatic in me though "That's so cool, I wish I could see!" though the woman with a baby head halfway out of her thought "Oh my god what???" With every contraction I pushed until I thought I was going to pass out. While the image of the woman on her back with her feet in the air stirs many negative feelings in the natural birth community, I really needed someone pushing my legs back like that. This baby just felt so big. Dr. Heiner said he did not want to cut an episiotomy but he would numb my perineum just in case. No scissors necessary, finally the head was out. I heard Dr. Heiner say to clamp the cord. I immediately knew this meant the baby had a very tight cord around its neck and it needed to be cut before the body could be born. As soon as I had the ok I began pushing as hard as I could. I wish I could have watched what was happening. One shoulder out, a doctor cursed, another shoulder, and I swear I pushed out every inch of that baby all the way to its toes. And at 6:48pm our baby was here! The emotional relief greatly outweighed the physical. Our baby was here. I was anxious to see who we had, a little boy or little girl, but before I could look someone said baby was having difficulty breathing, but really, baby wasn't breathing at all. I think Eric and I saw at the same time just as the nurse lifted baby off my chest. Eric said "We have another son!" He didn't yell it, it was just to me and it was so sweet to hear his excitement. The nurses resuscitate our son and when we finally got a glimpse our little boy was pink, but clearly struggling to breathe. My midwife called to me and reminded me to talk him and I did. His tummy was sucking in and he was wheezing loudly, it was nothing like when Milo had a little trouble breathing. The nurse said they might need to take him to the Neonatal Intensive Care Unit. His first APGAR score was 2, which is very low. He finally cried, three times, and they decided to have me try skin to skin instead of taking him away. His second APGAR was 8. It was a rough start but he was ok. I don't remember when they weighed him, before or after they gave him to me but when they did voices were raised in surprise and it took me a while to figure out what was happening... I think I may have been in the middle of pushing out the placenta. Eric finally told me, he weighed 11 pounds, 5 ounces! We were shocked! He was 21 3/4 inches with a 39 cm head and 39 cm chest. His head was the biggest our nurse had measured in 38 years. I didn't have any excessive bleeding, though I was given Pitocin right away, and had no tears! The placenta did not look aged by the way. I reminded the doctors that I wanted the placenta and I was told it had to go through pathology. I said we needed to get it home to clean because I was going to eat it. I suppose I forget how shocking fairly accepted behavior in the natural world is because the busy room froze. A nurse in the back said "What?!" I said I was going to have it encapsulated The looks of horror, disgust, and confusion were priceless. We were still not decided on a name. I liked Everett, Eric liked Indiana... yes after Indiana Jones. I was holding my ground on Everett but I had that night alone with the baby to think about it. I really liked our tradition of Eric naming our sons, which is Biblical. Eric also was amazing during the birth. He loved and supported me so much, and he may not have pushed out this baby himself but I'm certain I wouldn't have had the strength or confidence to do it without him. And honestly, if any baby deserved to be named Indiana, this one was it. We also kept our tradition of choosing a Hebrew middle name. Eric chose Jacob, which is also my grandmother's grandfather's name. So this is where I have to process this birth. I believe every birth is a lesson, which is one of the many reasons I take issue with routinely medicating and detaching women from their births. We are meant to trust birth. We are meant to learn from birth. But I realize that when I say that part of me sets birth apart as an outside entity. I know that there were several hours where I had already decided something was wrong but I didn't want to disrupt the birth process. There was me, and there was the birth. I put my design over my intuition, which is really one of the most important aspects of our design! It's easy to tell a woman to trust herself but when it's you that is in a very scary place and no one can tell you what is happening because no one can feel what you are feeling it's not so clear. I still don't completely understand why my labor progressed the way it did, however after researching and talking to other birth professionals I believe I had a spastic lower uterine segment, which is rare. I still believe this birth was meant for me. I came away with a new found respect for a mother's ability to read her baby and her body. Before a monitor could confirm it I knew my body and baby were not working together. I love natural birth. It never occurred to me that after experiencing a natural birth I'd then have a medicated one. If I did know that, I would assume that I'd mourn the birth I thought I would have... but I'm not. I support natural birth because it's what I believe is safest, but none of us, not even midwives, doulas, or childbirth educators, are guaranteed an uncomplicated birth. I'm going to be honest, it feels very weird to me that I can't say it was another natural birth, but that's just a title. It was a hard, complicated, scary day, but that doesn't mean it wasn't a good birth. I had a lot to learn and it was crammed it into an intense 12 hour lesson. I'm grateful for the experience, for the amazing team I had with me, the courageous doctors who could have easily justified a cesarean, for Eric's confidence in me, and for this sweet new baby boy, Indy. And yes... we know Indiana was the dog.
|
 I'm a childbirth educator, birth doula, and birth activist with 4 little boys and occasionally enough time to write. I'm a childbirth educator, birth doula, and birth activist with 4 little boys and occasionally enough time to write.
EventsNatural Birth Series
Sept 28 – Nov 15 Carmel, 6:30–9pm Register Infant Sleep for Expecting & New Parents September 28th 6:30pm - 9:00pm Register Gentle Cesarean: Planning & Recovery September 30th Toro Park, 3-6:30pm Register Natural Birth Refresher October 15th Salinas, 1– 4pm Register Preconception & Early Pregnancy Class October 22nd Salinas, 1– 4pm Register Sibling Prep for Parents & Kids November 4th & 5th Toro Park, 2:-4pm Register Fall Home & Birth Center Birth Series Nov 7 – Dec 12 Salinas 7pm–9pm Register VBAC Class November 12th Salinas, 1–4pm Register Natural Birth Series Nov 29th – Jan 17th Salinas 6:30–9pm Register Archives
January 2017
Categories
All
|