|
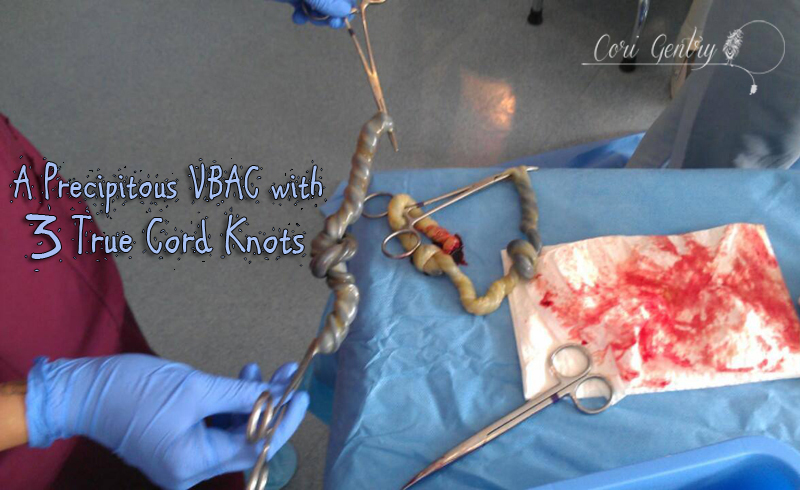
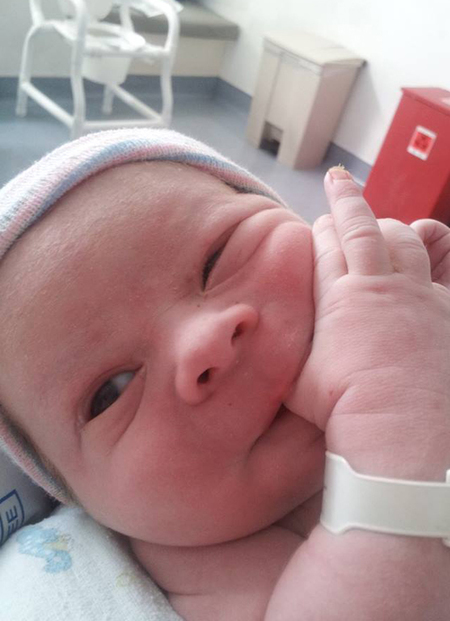
A Precipitous VBAC with 3 True Cord Knots Sara took my birth class while preparing for her second VBAC. She is an MD going into obstetrics so teaching Sara made for some interesting birth class moments... like... "so in the event of a c-section..." Sara: "oh yeah, when I do a c-section..." Haha oh yeah... you're a DOCTOR. I hope you enjoy the miraculous birth story of Sara's third baby, thank you for sharing it with us Sara! This is Raphe's Story We took our seats in church just as we do every Sunday. We’d been in a bit more of a hurry to get settled after running later than usual. This Sunday was my oldest daughter’s fifth birthday, and she’d spent most of the morning playing with her new toys and scarfing down chocolate chip pancakes. Getting dresses on and hair done had been particularly difficult, but I promised I’d help her build her new Lego set later that afternoon. As we sat down in the pew and started to sing the opening hymn, I felt a familiar tightening in my very swollen belly. Today was my due date, but I’d been having Braxton-Hicks contractions for weeks. I’d even had a few “false alarm” evenings when the contractions were particularly strong and increasingly regular. But nothing had panned out yet. I’d joked with A that she might get a baby brother for her birthday, but didn’t really think he’d come so predictably. By the time we were done with the song, the contraction was starting to subside. Twenty minutes later, the first speaker took the stand and another tightening started. And twenty minutes after that, another. Like clockwork, two or three more series of contractions happened every twenty minutes. My second baby, my first VBAC, had been what they call a “precipitous” delivery. I’d labored for about two hours with a transition of 15-20 minutes, 15 minutes of pushing, with five pushes total. I’d ended up with a perfect, VERY alert baby girl and a third-degree tear (this kid had flown out!). With my third, I was planning on delivering in Salinas at Natividad Medical Center despite living in Monterey (30 minutes to the Southwest), because the Community Hospital in Monterey Peninsula does not allow VBACs. Period. They are 100% b-a-n-n-e-d. I figured if this little guy was as precipitous as R had been, I’d better start heading toward the hospital as soon as I suspected active labor. My contractions had only been going on for a little over an hour, and they weren’t painful yet, but they were regular, strong, and getting more intense. I told my husband we’d better head out to the hospital just in case – better to be sent home than risk having the baby on the road! We left our two girls with some close friends who had planned on hosting them when the “big day” came. We grabbed our pre-packed bags and set out for the hospital. By the time we were halfway there, the contractions started getting intense enough to take my breath away. They still weren’t painful, just incredibly strong with a lot of pressure, and closer together. I was so glad the roads were clear and lights were green. If we’d attempted this drive during 5pm weekday rush-hour, I think I would have throttled the driver. At the sign-in desk, I had to stop talking during contractions and pace back and forth until they eased. Still no pain, but lots of pressure. Due to R’s quick delivery, the nurse completed my admission and showed us to our room. She took vitals, placed my hep-locked IV, and checked my cervix. I was dilated to 4 and 75% effaced at 0 station. Within 20 minutes my contractions had escalated from pressure to pain, and I used a birthing ball to moan my way through them. My husband let me hold on to his neck to take pressure off my belly, and I bounced slowly until the wave passed. During the next 20 minutes, the pain became impossible to “bounce” through, and I started throwing my upper body across the patient table (the one on wheels that they serve your meals on) and squatting down as close to the floor as possible. Stretching my body as long as possible was the best way for me to get through each increasingly intense crest of pain. I’m a pretty vocal laborer, and my nurse was very intuitive. She read my cues and decided to check me again – dilated to 7, 100% effaced. The pain gave way to intense pressure and the urge to push became unbearable. I asked her to check again within five minutes, as with R I’d gone from a 3 to 10 in less than 15 minutes. Sure enough, I was fully dilated. The doctor arrived (he was a hospital fellow on weekend call) and I started to push with each contraction. My water had still not broken and baby’s heart rate was starting to drop between pushes. They broke my water, but it took a few attempts – had they not done it manually I’m pretty sure he would have been born in the caul! I get pretty focused during the pushing phase, so I was only vaguely aware of what they were saying, but I could see the looks on their faces. “Meconium in the fluid.” “Late decelerations.” When they asked me to give him a break on the next contraction, I knew they were concerned for his well-being, and that if I didn’t get this kid out (and quick!), I’d be getting cut again. I tried to pause on the next contraction, but there was no stopping him. I knew he’d started crowning when I felt that familiar burning sensation, and I knew I could have him out with one more good push. They’d told me to wait again, but he was having none of it. Ten seconds later I felt the last rush of relief as his body slid out into the world. They’d warned me I wouldn’t hear him cry initially, that they wanted to suction him well before they stimulated a good, robust breath out of his lungs. I saw him only briefly before they took him to the warmer, and he looked bluish and floppy. He’d had a knot in his cord just above where they’d clamped and cut, which explained the disconcerting heart rate during delivery. I didn’t worry though – I just knew he was okay and wasn’t even remotely concerned. He would cry when he was good and ready – it was as if he was telling me this himself. After a minute of suction and stimulation, I heard his first little growl. It wasn’t a cry per se, but it was strong and reassuring. As soon as his heart rate and oxygen saturation were stable (about five minutes), they brought him to my chest and he began nursing vigorously. This kid was alert and ready for life! After I delivered the placenta, the doctor and nurses were astonished to find two more knots in his cord. That’s a grand total of three knots, three complete, true knots this kid had managed to tie in his cord. Now one knot increases the risk of infant mortality during delivery fourfold. This kid had THREE. Dr. Chandler would later tell me he’d never seen or heard of three cords in any medical literature, that my little guy might be a recorded first. But Raphe (short for Rapheal, from the Hebrew for “God has healed”) had absolutely no problems, no damage of any kind, no complications whatsoever. He was a nursing champ from the get-go and alert as a hawk. It didn’t hit me until much later what a blessing that was – with all that could have gone wrong, he had come to us, safe and sound, like some crazy Olympic gymnast with a perfect dismount. Raphe was 6 pounds 15 ounces and 19.5 inches long. I think the knots may have kept him from getting much bigger, because my girls (also full term) were 7 pounds 8 ounces and 22 inches, and 7 pounds 13 ounces and 22 inches. Raphe has grown over 5 inches in four months and now weighs 15 pounds.
We’d arrived at Natividad around 2:30 in the afternoon. Raphe was born at 3:17pm, so I’d labored for even less time than with R. Had we not left when we did, had we not packed and arranged childcare previously, had we hit traffic, had we delivered in the car on the side of the road next to a lettuce field, had we, had we, had we. . . We were truly watched over and blessed. I have no doubt Raphe is destined for great things, as I’m sure most parents feel about their children. If nothing else, with such a dramatic entrance into this world, I’m sure the next 18 years will be nothing if not entertaining.
1 Comment
Leave a Reply. |
 I'm a childbirth educator, birth doula, and birth activist with 4 little boys and occasionally enough time to write. I'm a childbirth educator, birth doula, and birth activist with 4 little boys and occasionally enough time to write.
EventsNatural Birth Series
Sept 28 – Nov 15 Carmel, 6:30–9pm Register Infant Sleep for Expecting & New Parents September 28th 6:30pm - 9:00pm Register Gentle Cesarean: Planning & Recovery September 30th Toro Park, 3-6:30pm Register Natural Birth Refresher October 15th Salinas, 1– 4pm Register Preconception & Early Pregnancy Class October 22nd Salinas, 1– 4pm Register Sibling Prep for Parents & Kids November 4th & 5th Toro Park, 2:-4pm Register Fall Home & Birth Center Birth Series Nov 7 – Dec 12 Salinas 7pm–9pm Register VBAC Class November 12th Salinas, 1–4pm Register Natural Birth Series Nov 29th – Jan 17th Salinas 6:30–9pm Register Archives
January 2017
Categories
All
|